Ultrasound Injections
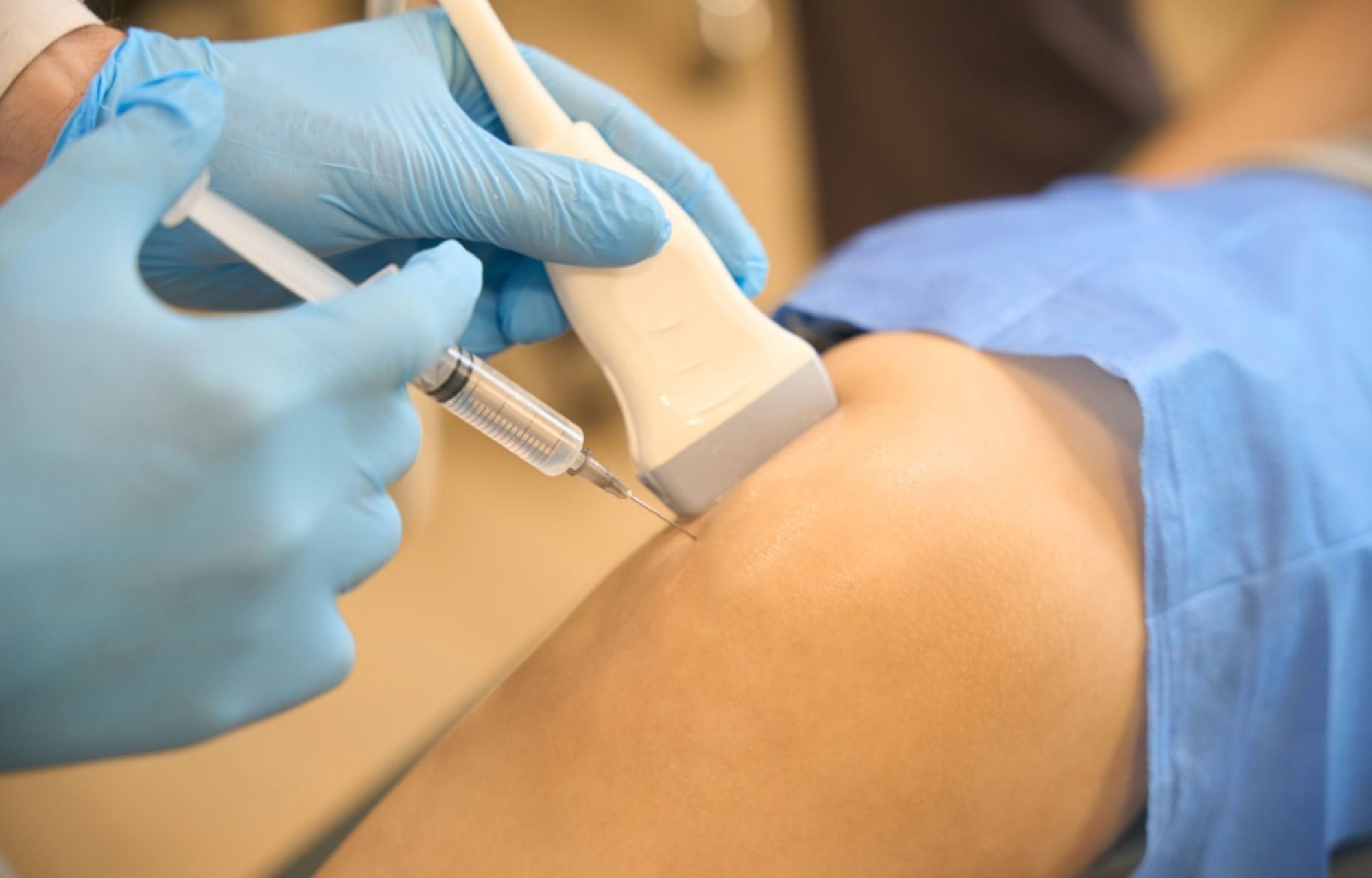
Ultrasound-guided steroid injections
Ultrasound-guided steroid injections deliver anti-inflammatory medication precisely to a painful or inflamed target (such as a joint, tendon, bursa, or near a nerve) using real-time ultrasound to improve accuracy and safety. The procedure is usually quick (around 10–20 minutes) and you can typically go home shortly afterwards; it generally involves:
Positioning and ultrasound imaging: gel and a probe are used to visualise the underlying structures.
Sterile preparation and needle guidance: the skin is cleaned, then a fine needle is advanced under live ultrasound to the exact site.
Injection: a corticosteroid (to reduce inflammation) often combined with a local anaesthetic (for immediate relief) is injected.
These injections are used to treat pain and inflammation in:
Joints: shoulder, knee, hip, ankle, wrist, elbow (including osteoarthritis and inflammatory arthritis).
Tendons/bursae: rotator cuff tendinitis, subacromial or trochanteric bursitis, trigger finger, De Quervain’s tenosynovitis, plantar fasciitis.
Nerve-related pain: carpal tunnel syndrome and other nerve entrapments.
They can also be used diagnostically if symptom relief helps confirm the source of pain. Key advantages of ultrasound guidance include improved accuracy versus “blind” injections, real-time confirmation of needle placement, reduced risk to nearby nerves/blood vessels/tendons, and often better results for small or deep structures. After the injection, temporary numbness for a few hours and mild soreness are common; steroid relief typically begins within 2–7 days and may last weeks to months. Uncommon risks include a short-lived pain flare, rare infection, skin thinning or colour change at the site, temporary rise in blood sugar, and (with repeated injections) possible weakening of tendons or cartilage—overall making this a safe, minimally invasive option when rest, physiotherapy, or medication haven’t been enough.
Ultrasound Guided Hyaluronic Acid Injections
We are an approved ostenil injection clinic.
Within every healthy joint there is protective cartilage and synovial fluid.
With increasing wear and tear, the cartilage becomes worn down and the bones can become damaged. Within the synovial fluid is a substance called hyaluronic acid, and it’s the key for maintaining healthy joints. It is a type of glycosaminoglycan, which is a long chain of sugars that helps to retain water and promote lubrication to joints. By injecting it into the cavity around the joint it can slow the breakdown of synovial fluid. This means it can decrease your symptoms and alleviate the pain and stiffness associated with osteoarthritis.
Each course of natural injection therapy can provide relief for up to 9 months or longer.
Hyaluronic acid (HA) joint injections, also called viscosupplementation, are commonly used to treat osteoarthritis, especially in the knee, though they may also be used in the hip, shoulder, or ankle in some cases.
How It Works:
In osteoarthritis, HA levels decrease, making joints stiff and painful. Injections aim to restore the viscosity of the joint fluid to improve mobility and reduce pain.
Common Uses:
Knee osteoarthritis (most common and FDA-approved)
Early to moderate stages of Osteoarthritis (may be less effective in severe OA)
For patients who don’t respond well to NSAIDs or physical therapy
As a non-surgical option before considering joint replacement
Potential Benefits:
Reduced joint pain
Improved mobility and function
Delayed need for surgery
Generally well tolerated
Limitations:
Relief may take a few weeks to notice
Effects may last 6-9 months, but vary by individual
Not effective for everyone
Not a cure—it’s a symptom management tool
Risks (generally low):
Temporary joint swelling or pain at the injection site
Rare allergic reaction or infection
Post-injection flare
Prolotherapy
Why prolotherapy is considered for tendinopathy
Chronic tendinopathy usually involves:
Collagen degeneration
Poor blood supply
Minimal true inflammation
Prolotherapy aims to:
Stimulate a healing response at the tendon–bone junction (enthesis)
Encourage collagen remodeling and tendon strengthening
Improve pain and function over time
Common tendinopathies treated
Lateral epicondylitis (tennis elbow)
Medial epicondylitis (golfer’s elbow)
Achilles tendinopathy
Patellar tendinopathy (jumper’s knee)
Rotator cuff tendinopathy
Arthrosamid injections
Arthrosamid is an injectable, non-biodegradable hydrogel primarily composed of water. It is designed to treat knee osteoarthritis by providing a cushioning effect within the joint. When injected, it integrates into the synovial membrane, creating a flexible, shock-absorbing layer that reduces friction, pain, and inflammation.
Benefits of Arthrosamid Injections
Pain Relief: Many patients experience significant pain reduction shortly after the injection, with maximum benefits often felt within a few weeks.
Improved Mobility: By cushioning the joint, Arthrosamid can enhance knee function, allowing individuals to return to daily activities more comfortably.
Minimally Invasive: The procedure is quick, typically lasting about 15-30 minutes, and patients can usually resume light activities the same day.
Long-lasting Effects: Arthrosamid can provide relief for several years, often delaying the need for more invasive procedures like knee replacement surgery.
Procedure and Effectiveness
The injection is performed under local anesthesia in a clinical setting. Patients may feel some discomfort at the injection site, but serious side effects are rare. Clinical studies indicate a high success rate, with over 70% of patients reporting significant improvements in pain and mobility./
Considerations
Not for Everyone: Arthrosamid is intended for individuals with mild to moderate knee osteoarthritis and is not suitable for those with severe arthritis or inflammatory conditions like rheumatoid arthritis.
Potential Side Effects: Common side effects include mild pain, bruising, or swelling at the injection site, which typically resolve quickly.
In summary, Arthrosamid injections offer a promising non-surgical option for managing knee osteoarthritis, helping to alleviate pain and improve quality of life for many patients. If you are considering this treatment, consult with a healthcare provider to determine if it is suitable for your condition.
Ready to speak to us?

